 By Gazette Staff By Gazette Staff
May 13th, 2026
BURLINGTON, ON
The Joseph Brant Museum eat make share speaker series, featuring acclaimed Canadian cookbook authors.
Each month, a new speaker will discuss their publication and how their family’s cultural background has influenced their culinary journey. Attendees will also enjoy a recipe demonstration and have the opportunity to view the special exhibit eat make share: a taste of immigration from the Canadian Museums of Immigration at Pier 21. Featured titles will also be available for purchase directly from the author and in the Museum’s gift shop.
Ticket includes admission to Joseph Brant Museum, speaker presentation (7pm), and light refreshments. The Museum will open 1-hour prior to the presentation at 6pm for those who wish to view the special exhibit eat make share: a taste of immigration. This event is recommended for ages 12+.
May 26, 2026 | My Cypriot Table by Irene Matys
 Irene Matys is a World Gourmand Award winning and Globe and Mail bestselling cookbook author, television food expert, and farm-to-table advocate. She is the author of My Cypriot Table: Mediterranean Recipes for Gathering, Sharing, and Savouring, a celebrated debut cookbook featuring over 100 vibrant recipes inspired by her Greek Cypriot heritage and Canada’s seasonal bounty. Irene Matys is a World Gourmand Award winning and Globe and Mail bestselling cookbook author, television food expert, and farm-to-table advocate. She is the author of My Cypriot Table: Mediterranean Recipes for Gathering, Sharing, and Savouring, a celebrated debut cookbook featuring over 100 vibrant recipes inspired by her Greek Cypriot heritage and Canada’s seasonal bounty.
Born in Cyprus, Irene immigrated to Canada in 1976 as a refugee, bringing with her a deep rooted connection to food, family, and tradition. Her culinary journey began early, spending much of her childhood in her parents’ restaurant, Ciccio’s Pizza, which they purchased in Sarnia in 1980. Alongside this experience, it was her mama, her yiayia ( grandmother), and the family garden that truly nurtured her love of cooking, instilling in her the importance of fresh, seasonal ingredients and the joy of sharing meals. A committed advocate for community-focused food education, Irene designs culinary experiences that celebrate sustainability, cultural heritage, and connection.
Tickets: HERE

 By Gazette Staff By Gazette Staff
March 18th, 2026
BURLINGTON, ON
The Ontario Hospital Coalition has been fighting the good fight to keep health care services public.
Hundreds came out to their call on the federal Liberal MPs to help stop Alberta & Ontario’s privatization,.

 On Monday March 16, people across Canada rallied outside the offices of their local Liberal Members of Parliament in a nationwide Day of Action to warn that public health care for all in Canada is under unprecedented threat and to call on the federal government to enforce the Canada Health Act. The Ontario Health Coalition held seven events in Ontario in Ajax, Hamilton, London, Peterborough, Toronto and Waterloo — and one more is coming up in Kingston on Friday, March 20 at the Hon Mark Gerretsen’s office at 234 Concession St. On Monday March 16, people across Canada rallied outside the offices of their local Liberal Members of Parliament in a nationwide Day of Action to warn that public health care for all in Canada is under unprecedented threat and to call on the federal government to enforce the Canada Health Act. The Ontario Health Coalition held seven events in Ontario in Ajax, Hamilton, London, Peterborough, Toronto and Waterloo — and one more is coming up in Kingston on Friday, March 20 at the Hon Mark Gerretsen’s office at 234 Concession St.
The Key Issues:
Alberta’s Danielle Smith government has launched an unprecedented frontal assault on the Canada Health Act to end single tier Public Medicare. The law brings in private for-profit health insurance like they have in the U.S., enables physicians to charge patients for care, brings in queue jumping for the wealthy pushing everyone else back in line, and more. It is not “like” U.S. style health care. It is U.S. private health care, and for-profit health care interests are lined up to cash in.
Closer to home, Ontario’s Premier Doug Ford is privatizing public hospitals and is allowing private clinics to charge patients thousands for needed care. By the government’s own numbers, their latest set of private clinics (some of which are essentially hospitals, a number of which are chain owned) aim to redirect 1.2 million patients away from public hospitals. While the government is giving hundreds of millions more to private clinics, it has pushed the majority of public hospitals into deficit in a direct transfer of public resources. Patients are already being charged more than $4,000 per eye in the private cataract surgery clinics that Ford brought in, in violation of our medicare protection laws.

 By Gazette Staff By Gazette Staff
Mar 17, 2026
BURLINGTON, ON
Legal action follows public health warning about infection control practices at Burlington clinic
Diamond and Diamond Lawyers have filed a $5 million lawsuit in the Ontario Superior Court of Justice on behalf of Burlington resident Darwin Allen, who allegedly contracted Hepatitis C after being injected with an unsterile needle during treatment at the Halton Family Health Centre Walk-In Clinic.
The lawsuit names Halton Family Health Centre Inc. and Dr. Timothy Salter as defendants and alleges negligence, vicarious liability and breach of fiduciary duty.
According to the Statement of Claim, Mr. Allen attended the clinic in September 2023 after suffering a cut to his heel. During treatment, Dr. Salter allegedly injected him with lidocaine using an unsterile needle.
 In November 2025, Mr. Allen received a letter from Halton Region Public Health advising that improper infection prevention and control practices involving the use of unsterile needles with multidose vials of anesthetic medication had been identified at the clinic. The letter advised him to consult his healthcare provider and undergo testing for Hepatitis B, Hepatitis C and HIV. In November 2025, Mr. Allen received a letter from Halton Region Public Health advising that improper infection prevention and control practices involving the use of unsterile needles with multidose vials of anesthetic medication had been identified at the clinic. The letter advised him to consult his healthcare provider and undergo testing for Hepatitis B, Hepatitis C and HIV.
Shortly thereafter, Mr. Allen underwent a Hepatitis C blood test. In December 2025, he was notified that he had tested positive for Hepatitis C.
“No patient should walk into a clinic for routine treatment and leave with a life-altering infection,” said Darryl Singer of Diamond and Diamond Lawyers. “This case is about accountability and ensuring proper medical standards are followed.”
 The lawsuit alleges the defendants breached their duty of care by failing to implement appropriate infection prevention and control measures and failing to ensure needles used in treatment were properly sterilized. The lawsuit also alleges Halton Family Health Centre Inc. is vicariously liable for the conduct of Dr. Salter. The lawsuit alleges the defendants breached their duty of care by failing to implement appropriate infection prevention and control measures and failing to ensure needles used in treatment were properly sterilized. The lawsuit also alleges Halton Family Health Centre Inc. is vicariously liable for the conduct of Dr. Salter.
Diamond and Diamond Lawyers believe Mr. Allen may not be the only patient affected. Individuals treated at the Halton Family Health Centre Walk-In Clinic who later received a public health notice, or who have concerns about their care, are encouraged to contact the firm.
Diamond and Diamond Lawyers is a Canadian personal injury and medical negligence law firm that has recovered over a billion dollars in settlements for injured Canadians.
Related news story:
Resident found that he was infected after attending a clinic that had used needles that were not properly sterilized

 By Lori Croonen By Lori Croonen
February 18th, 2026
BURLINGTON, ON
Food is one of the most powerful choices we make every day. It shapes our energy, resilience, and long-term health. Choosing a vegan diet — whether for ethical, environmental, or personal reasons — can also be a meaningful way to support physical wellbeing.
At its foundation, vegan eating centers on plant foods: vegetables, fruits, legumes, whole grains, nuts, and seeds. These foods are rich in fiber, antioxidants, vitamins, minerals, and protective plant compounds known as phytonutrients. Together, these nutrients help reduce inflammation, support immune function, and promote healthy aging.
 Plant foods provide heart-supportive nutrients such as potassium, magnesium, and healthy unsaturated fats from nuts and seeds. One of the most important health advantages of a vegan diet is fiber intake. Fiber exists only in plant foods and plays a critical role in digestive health, blood sugar balance, and heart health. Adequate fiber consumption is associated with lower risks of cardiovascular disease, type 2 diabetes, and certain cancers. Because animal products contain no fiber, shifting toward plant-based meals naturally increases this essential nutrient.
Plant-based eating patterns are also typically lower in saturated fat and contain no dietary cholesterol. High intake of saturated fat and cholesterol — commonly found in red and processed meats — has been linked to increased risk of heart disease. In contrast, plant foods provide heart-supportive nutrients such as potassium, magnesium, and healthy unsaturated fats from nuts and seeds.
Even when comparing processed options, there are distinctions worth noting. Processed plant-based alternatives generally contain no cholesterol and are often lower in saturated fat than traditional processed meats. Processed meats have been classified as carcinogenic to humans due to their association with colorectal cancer. Plant-based alternatives do not carry that same classification, and they may still provide fiber and beneficial plant compounds absent in animal-based products.
Vitamin B12 is often raised in discussions about vegan nutrition. B12 is produced by bacteria — not by plants or animals. Historically, humans obtained B12 through soil exposure and animal foods. In modern food systems, many farmed animals are supplemented with B12 because they are not grazing naturally, meaning consumers are often receiving supplemented B12 indirectly. Importantly, B12 deficiency is not limited to vegans; many people, especially older adults or those with absorption issues, can have low levels regardless of diet. For vegans, using fortified foods or a simple supplement is a safe and reliable way to meet needs.
A well-planned vegan diet can provide adequate protein from legumes, tofu, tempeh, whole grains, nuts, and seeds. Iron is available from beans and lentils, particularly when paired with vitamin C-rich foods to enhance absorption. Calcium can be found in fortified plant milks and leafy greens.
 Choosing vegan is not about restriction; it is about intention. Choosing vegan is not about restriction; it is about intention. It encourages building meals around nutrient-dense plant foods that support cardiovascular health, digestive wellness, and metabolic balance. Whether someone adopts it fully or simply increases plant-based meals, emphasizing plants over animal products can significantly improve overall dietary quality.
In a time when chronic diet-related illnesses are widespread, vegan eating offers a proactive, evidence-informed approach to nourishment — one that supports long-term health while empowering individuals to make conscious choices about how they feed themselves.
Burlington Vegfest 2026 on August 15th at Spencer Smith Park!    

 By Gazette Staff By Gazette Staff
February 4th, 2026
BURLINGTON, ON
Wine for Friends, a signature fundraising event hosted by Rotary Burlington Lakeshore took place this evening.
The occasion was used by the Rotary Burlington Lakeshore to formally announce a $200,000 pledge to the Joseph Brant Hospital Foundation in support of the For All Minds Mental Health & Addictions Campaign.
Why This Matters
Mental health and addictions services continue to see rising demand across Burlington and Halton Region. This $200,000 pledge represents one of Rotary Burlington Lakeshore’s most significant investments in local healthcare and underscores the power of community-led philanthropy.

 By Gazette Staff By Gazette Staff
February 2nd, 2026
BURLINGTON, ON
Frailty has been described as one of the most problematic expressions of population ageing. However, frailty screening isn’t done as part of standard medical care.
A new made-in-Hamilton app is helping health-care providers identify the risk of frailty and age-related loss of muscle mass and strength in less than 15 minutes. The Fit-Frailty App – developed at the Geras Centre for Aging Research, a Hamilton Health Sciences (HHS) research centre funded by HHS and affiliated with McMaster University – is the only comprehensive frailty assessment app of its kind.
The Geras team worked with the HHS Centre for Data Science and Digital Health (CREATE) team who works with hospital clinicians to develop new ideas and create digital solutions that fundamentally reimagine how health care is delivered.
 Dr. Courtney Kennedy, a Hamilton Health Sciences and McMaster researcher and an occupational therapist. “The Fit-Frailty app is a more holistic measure as it looks at several different aspects that contribute to a patient’s frailty level including physical, cognitive and mental health,” says Dr. Courtney Kennedy, a Hamilton Health Sciences and McMaster researcher and an occupational therapist who led the development of the Fit-Frailty app. “Understanding not only how frail someone is but also identifying areas where intervention is needed can help doctors and other clinicians better assess a patient’s level of frailty and develop individualized care plans.”
Currently, the app has been piloted in clinical practice at Hamilton Health Sciences and with the McMaster Division of Rheumatology led by Dr. Arthur Lau and Dr. Jonathan (Rick) Adachi. It is also being used in three large CIHR-funded clinical trials led by GERAS and the McMaster Division of Rheumatology.
There have been approximately 500 research participants thus far and the team plans to provide further launch and knowledge translation in the future.
The study testing the Fit-Frailty App has recently been published in the British Medical Journal (BMJ) at https://bmjopen.bmj.com/content/15/12/e098892.full.
“We were able to demonstrate that slow-paced rehabilitation at Hamilton Health Sciences is an effective program for reducing frailty and improving function,” says Kennedy. “One of the most novel elements of this App is that we were able to show that it could be used to measure intervention change for pre- and post-rehabilitation.”

 By Gazette Staff By Gazette Staff
January 26th, 2026
BURLINGTON, ON
A new report warns that the turn to health care cutbacks in Ontario harken to the period of Mike Harris, as hundreds of job cuts ravage hospitals across the province, prolonging wait-times and delaying patient care.
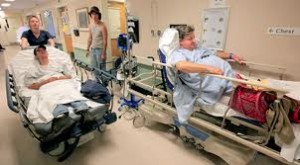 What will wait times look like with staffing cuts? The government recently directed hospitals to plan for two per cent annual funding increases until 2027-28 – far less than the six per cent average in recent years – precipitating job cuts at Hamilton Health Sciences and St. Joseph’s Healthcare.
“The Ford government’s funding plan will lead to more than 10,000 job losses and reduction of 2,400 hospital beds across the province at a time when 2,000 patients are receiving “hallway healthcare” every day, says the report by the Ontario Council of Hospital Unions, the hospital division of CUPE.
Driven to the brink: projected cuts to intensify hospital crisis will be released at a press conference in Hamilton at 2 p.m.
The report uses data on hospital staffing, capacity and funding from multiple official sources, and offers recommendations to address patient needs and restore lost capacity in the sector.
On Tuesday, the union will reveal the projected staffing and hospital bed cuts in Hamilton through to 2027-28, and contrast that with the number of beds required to maintain current service levels.

 By Gazette Staff By Gazette Staff
January 16th, 2026
BURLINGTON, ON
The Ontario government is investing up to $8 million to support planning for 16 new and expanded primary care teaching clinics across the province to connect 300,000 more people to primary care. This investment is part of the government’s $2.1 billion Primary Care Action Plan to connect everyone in Ontario to primary care by 2029.
 The development of skills to effectively work with patients takes time and proper funding. “These new primary care teaching clinics will further protect our health-care system by training the next generation of primary care clinicians, right here in Ontario,” said Sylvia Jones, Deputy Premier and Minister of Health. “This builds on our government’s unprecedented investments in primary care that will ensure anyone who wants to connect to a primary care clinician can have reliable access to primary care, no matter where they live.”
Each teaching clinic will receive up to $500,000 to support planning work. In partnership with Ontario’s medical schools, these clinics will train family medicine residents in a team-based model alongside other health-care professionals, such as nurse practitioners, physician assistants and registered nurses. These clinics will offer training that combines direct patient care with hands-on learning in team-based environments, all while providing primary care for an additional 300,000 people. Initial teaching clinics are targeted to open in 2027-28, with further expansion to follow.
“Hands-on learning is critical to ensuring our health care students can hit the ground running and provide exceptional care upon graduation,” said Nolan Quinn, Minister of Colleges, Universities, Research Excellence and Security. “The new and expanded primary care clinics will not only equip our future doctors and nurses with the skills they need to thrive, but also connect more people in Ontario to compassionate health care, close to home.”
This funding is part of the government’s broader investment of up to $300 million – part of the $2.1 billion Primary Care Action Plan – to build new and expanded community-based primary care teaching clinics in areas with high rates of unattachment. In addition to funding planning grants for 16 new and expanded teaching clinics, two new primary care teaching clinics at Toronto Metropolitan University will bring the total to 18 clinics. Together with other historic investments in new medical school seats, creating over 130 new and expanded primary care teams and adding nearly 20,000 new physicians to the health-care system, these initiatives are helping to connect Ontario families to primary care, beginning with clearing the Health Care Connect waitlist as of January 1, 2025. As of this week, that waitlist has been reduced by more than 75 per cent.
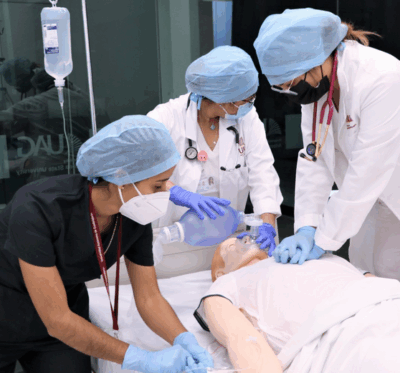 Investment in critical infrastructure will strengthen team-based primary care in Ontario. “This investment in critical infrastructure will strengthen team-based primary care in Ontario,” said Dr. Jane Philpott, Chair of Ontario’s Primary Care Action Team. “These new teaching clinics will train the next generation of family physicians, nurse practitioners, physician assistants and other health professionals to work in teams while delivering vital care to patients who currently lack access.”
| Medical school |
Primary Care Teaching Clinic Site Location |
| McMaster University |
Milton |
| McMaster University |
Niagara |
| NOSM University |
Thunder Bay |
| NOSM University |
Sudbury |
| NOSM University |
Sault Ste. Marie |
| NOSM University |
Timmins |
| NOSM University |
North Bay |
| Queens University |
Oshawa |
| Queens University |
Kingston |
| Queens University |
Belleville |
| University of Ottawa |
Central Ottawa |
| University of Toronto |
Scarborough (two sites) |
| Western University |
London East |
| Western University |
Sarnia |
| Western University |
Woodstock |
Through Your Health: A Plan for Connected and Convenient Care, the Ontario government continues to take bold and decisive action to grow the province’s highly skilled health-care workforce and ensure people and their families have access to high-quality care, closer to home, for generations to come.
There is a lot of fluff in the provincial government’s announcement, but the fact that this program is now real and live is good news.

 By Gazette Staff By Gazette Staff
January 15th, 2026
BURLINGTON, ON
Hamilton Health Sciences advises that “It’s likely that community members are digging themselves out after the recent snow fall and this means that hospitals may see an increase in the number of individuals experiencing serious heart attacks.
 “Statistically, we see a rise in heart attacks and heart-related deaths after significant snowfalls,” says Dr. Craig Ainsworth, Cardiology and Chief of Critical Care at Hamilton Health Sciences’ Hamilton General Hospital (HGH). “Repeatedly lifting heavy snow causes your heart rate to increase and blood pressure to rise considerably. For some people, especially those with certain risk factors, this can lead to a heart attack.” “Statistically, we see a rise in heart attacks and heart-related deaths after significant snowfalls,” says Dr. Craig Ainsworth, Cardiology and Chief of Critical Care at Hamilton Health Sciences’ Hamilton General Hospital (HGH). “Repeatedly lifting heavy snow causes your heart rate to increase and blood pressure to rise considerably. For some people, especially those with certain risk factors, this can lead to a heart attack.”
Those with known heart disease, people who are sedentary, and those middle-aged or older are at higher risk. Ainsworth advises people at risk to ask a friend or neighbour for help, use a smaller shovel to lighten the load or, if possible, invest in a snow blower.
 If you must shovel, be mindful of heart attack warning signs. If you must shovel, be mindful of heart attack warning signs, which can vary significantly from person to person. Some people may experience pain in their neck and shoulder, while others become nauseous and light-headed.
Wide-ranging symptoms can include:
• Chest discomfort such as pressure, squeezing, fullness, pain, burning or heaviness
• Upper body discomfort in the neck, jaw, shoulder, arms or back
• Tingling or numbness
• Nausea and vomiting
• Dizziness
• Sweating
• Shortness of breath
• Feeling of the heart pounding
• Indigestion
• Feeling faint or anxious
Follow these steps if you or someone nearby has symptoms:
• Call 9-1-1
• Stop all activity and sit or lay down
• If you have nitroglycerin, take your prescribed dose
• Take Aspirin. Chew and swallow one 325 mg or two 81 mg tablets
• Rest and wait for help to arrive
For additional snow shoveling safety tips, please visit https://www.hamiltonhealthsciences.ca/share/snow-shoveling/.

 By Gazette Staff By Gazette Staff
November 10th, 2025
BURLINGTON, ON
This is not something Canada should be proud of.
 The measles outbreak in Canada and how we reacted to it has resulted in the Pan American Health Organization (PAHO) advising the The Public Health Agency of Canada that it has lost its measles elimination status — a designation it has held since 1998. The measles outbreak in Canada and how we reacted to it has resulted in the Pan American Health Organization (PAHO) advising the The Public Health Agency of Canada that it has lost its measles elimination status — a designation it has held since 1998.
PHAC said it is collaborating with the PAHO and working with the federal, provincial, territorial and community partners to implement co-ordinated actions. These include focusing on “improving vaccination coverage, strengthening data sharing, enabling better overall surveillance efforts, and providing evidence-based guidance,” the statement said.
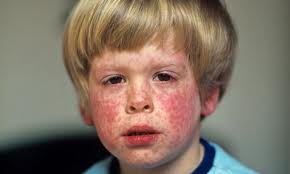 A severe case of measles. Canada has recorded more than 5,100 measles cases this year, the majority tied to the multi-province outbreak, according to the most recent federal data.

 By Pepper Parr By Pepper Parr
October 1st, 2025
BURLINGTON, ON
There will soon be more older people than young people in the city.
And many of those older people are going to need levels of care that are not normally provided.
 University Professor Tim O’Connell, Chair of Recreation and Leisure Studies at Brock University explains that: “As society increasingly embraces a holistic approach to health, recreation has emerged at the critical intersection of personal wellness and community well-being. University Professor Tim O’Connell, Chair of Recreation and Leisure Studies at Brock University explains that: “As society increasingly embraces a holistic approach to health, recreation has emerged at the critical intersection of personal wellness and community well-being.
To meet the growing demand for skilled professionals in recreation fields, Brock University and Mohawk College have signed two transfer pathway agreements to deliver flexible options for students to pursue either a Bachelor of Therapeutic Recreation or Bachelor of Recreation and Leisure Studies.
The articulation agreements set students on a direct track from Mohawk College’s two-year Recreation Therapy and 16-month Accelerated stream programs to either Brock program. Eligible students will receive a block of seven transfer credits, fast-tracking them toward their 20-credit degree.
By embedding courses such as Leisure Education in Therapeutic Recreation in a broader recreation and leisure studies framework, Brock’s programs equip graduates with in-demand skills, professional experience and industry-recognized credentials. Career paths range from clinical practice in hospitals and long-term care facilities to community-based roles where recreation and leisure contribute to physical, social and emotional well-being.
 The Therapeutic Recreation program also qualifies students to participate in the National Council for Therapeutic Recreation Certification. “The pathways are a game-changer for students,” says Connell. “They not only gain advanced standing in their degree but increase their career readiness by graduating with an essential credential employers are looking for in hospitals, long-term care facilities and treatment centres.”
In addition to clinical practice, students complete a 560-hour supervised internship, benefit from access to an extensive alumni network and have options to pursue an honours thesis.
The Therapeutic Recreation program also qualifies students to participate in the National Council for Therapeutic Recreation Certification (NCTRC) exam, a credential increasingly sought by employers across Canada and the United States.

 By Gazette Staff By Gazette Staff
September 17th, 2025
BURLINGTON, ON
The Region issued a report yesterday on problems at the Halton Family Health Centre Walk-in Clinic located at 2951 Walkers Line where needles were improperly used on occasions where a local freezing was being applied.
The original report said:
Following an investigation, Halton Region Public Health identified improper infection prevention and control practices involving the use of an unsterile needle with a multidose vial of local anesthetic medication (freezing) between January 1, 2019, and July 17, 2025. This practice may pose a risk of cross-contamination and transmission of infections. The investigation determined this was likely not an isolated incident, meaning it may have occurred previously during the identified time period between 2019 and 2025. This IPAC Lapse only includes the walk-in clinic during the specified time period and does not include procedures or care received at the family practice physician offices associated with the Halton Family Health Centre clinic.
Halton Family Health Centre Walk-in Clinic has taken immediate corrective measures to ensure all necessary infection control measures are being met. Public health continues to monitor the situation to ensure compliance and patient safety. There are no risks to the patients at this time, and the clinic is open.
The Region has since updated the report to say:
 This public notice has been updated to provide clarity and ensure an accurate understanding of the infection prevention and control lapse. It is important to note that the same needle was not used continuously throughout the period, rather appropriate infection prevention and control measures were not followed when using multi does vials over the time period identified. This public notice has been updated to provide clarity and ensure an accurate understanding of the infection prevention and control lapse. It is important to note that the same needle was not used continuously throughout the period, rather appropriate infection prevention and control measures were not followed when using multi does vials over the time period identified.
While the risk remains low, Halton Region Public Health continues to encourage anyone who visited the walk-in clinic during the specific timeframe and received a needle for the purposes of “freezing”, to seek precautionary testing and speak with their healthcare provider.

 By Gazette Staff By Gazette Staff
September 17th, 2025
BURLINGTON, ON
Public Notice: Infection Prevention and Control (IPAC) Lapse at Walk-In Clinic in Burlington
 Halton Region Public Health is notifying the public of an infection prevention and control (IPAC) lapse at the Halton Family Health Centre Walk-in Clinic located at 2951 Walkers Line in Burlington (corner of Walkers Line and Dundas Street). Halton Region Public Health is notifying the public of an infection prevention and control (IPAC) lapse at the Halton Family Health Centre Walk-in Clinic located at 2951 Walkers Line in Burlington (corner of Walkers Line and Dundas Street).
Halton Region Public Health investigation
Following an investigation, Halton Region Public Health identified improper infection prevention and control practices involving the use of an unsterile needle with a multidose vial of local anesthetic medication (freezing) between January 1, 2019, and July 17, 2025. This practice may pose a risk of cross-contamination and transmission of infections. The investigation determined this was likely not an isolated incident, meaning it may have occurred previously during the identified time period between 2019 and 2025. This IPAC Lapse only includes the walk-in clinic during the specified time period and does not include procedures or care received at the family practice physician offices associated with the Halton Family Health Centre clinic.
Halton Family Health Centre Walk-in Clinic has taken immediate corrective measures to ensure all necessary infection control measures are being met. Public health continues to monitor the situation to ensure compliance and patient safety. There are no risks to the patients at this time, and the clinic is open.
Important instructions for patients of the Halton Family Health Centre Walk-in Clinic
Patients who visited the Halton Family Centre Walk-in Clinic between January 1, 2019 and July 17, 2025, and received a treatment requiring local anesthetic by injection (freezing) may have been exposed to blood and blood-borne infections. Examples of procedures that may require local anesthetics include but are not limited to:
- laceration repairs (stitches for cuts or tears of the skin)
- intrauterine Device (IUD) insertions
- endometrial biopsies
- skin biopsies
- removal of lumps and bumps
- partial or complete nail removal
- joint injections or aspirations
Although the risk of infection is low, Halton Region Public Health is advising patients who received a procedure that may require local anesthetic by injection (freezing) at the Halton Family Health Centre Walk-in Clinic between January 1, 2019, and July 17, 2025 to:
- speak with their healthcare provider or visit a walk-in clinic to discuss testing for hepatitis B, hepatitis C, and HIV
- download and print a copy of the laboratory requisition and physician letter to bring to the healthcare provider
- not visit a hospital emergency department, as it is not necessary
“Protecting the health and safety of the public and patients is a top priority. Our Public Health team continues to actively monitor the situation and ensure compliance is maintained,” said Dr. Deepika Lobo, Medical Officer of Health for Halton Region. “While the risk of transmission is low, we are ensuring impacted individuals have the information they need to complete precautionary testing.”
To learn more about this IPAC lapse, please visit the IPAC Lapse Disclosure webpage.
Patients of the clinic who have specific questions about the lapse are asked to call Halton Region Public Health at 311, 905-825-6000 or toll-free 1-866-442-5866

 By Diana Kharchenko By Diana Kharchenko
September 17th, 2025
BURLINGTON, ON

Researchers in multiple countries are advancing stem cell trial research aimed at repairing the inner ear to restore hearing in people with tinnitus and neural hearing loss. The initial research investigations aim to determine if cochlear hair cells, which transform sound into brain signals, can be regenerated.
The 2022 JAMA Neurology review established that tinnitus impacts 14.4% of adults worldwide, resulting in more than 740 million cases, while severe tinnitus affects 2.3% of the population (JAMA Neurology). The available treatments, including hearing aids and cochlear implants, and sound therapy, provide symptom relief, but they cannot restore typical hearing function.
Researchers at Harvard Medical School’s Mass Eye and Ear used a drug-like cocktail to stimulate hair cell regeneration in mice, which shows promise for human clinical applications.
Dr. Zheng-Yi Chen from Harvard Medical School’s Otolaryngology-Head & Neck Surgery department described hair cell regeneration in the inner ear as the ultimate goal of hearing research. The research shows that clinical applications are possible for the future (Harvard Medical School).
Advances in Regenerative Research
Tinnitus and many forms of neural hearing loss result from damage to cochlear hair cells or their neural connections. The therapy with mesenchymal stem cells (MSCs) works to establish a supportive environment for the body’s repair mechanisms by delivering growth factors and enhancing immune responses and microcirculation.
Traditional treatments, including hearing aids and cochlear implants, and medications, help millions of people, but they cannot fix the complete damage to the ear.
Dr. Chris Cunningham from the University of Pittsburgh (Eye & Ear Foundation) explained that these devices bring revolutionary life-changing benefits, yet they cannot restore normal hearing completely.
Many stem cell trial programs now focus on MSCs, adult multipotent stromal cells sourced from a patient’s tissue or donated placental and umbilical cord tissue. MSCs avoid the ethical concerns associated with embryonic stem cells and have a lower risk of immune rejection.
According to reviews in Frontiers in Cellular Neuroscience (Warnecke et al., 2021) and Molecular Biology Reports (2020), MSCs have been shown to reduce inflammation, protect nerve cells, repair synaptic connections, and promote new blood vessel growth to improve circulation.
Global and Clinical Perspectives
 Scientists throughout the world continue to study cell-based hearing loss treatments in laboratories and clinics because they share a common goal of developing treatments that surpass symptom relief. Beyond university laboratories, some private clinics are also exploring regenerative approaches for tinnitus and neural hearing loss. The European clinic Swiss Medica operates among multiple facilities that provide stem cell therapy for tinnitus through MSCs. The clinic explains that these treatments work to decrease inflammation while defending auditory nerve structures and promoting tissue regeneration.
The U.S. medical institution AdventHealth initiated a Phase I/II clinical trial to evaluate autologous umbilical cord blood infusion for treating acquired hearing loss in children while focusing on safety and practicality. The MHRA granted approval to Rinri Therapeutics in 2025 for starting human trials of Rincell-1, which functions as a regenerative cell therapy to fix damaged auditory nerves.
Scientists throughout the world continue to study cell-based hearing loss treatments in laboratories and clinics because they share a common goal of developing treatments that surpass symptom relief.
Future Outlook
While early results are encouraging, experts emphasise that stem cell therapies for hearing disorders remain experimental.
According to a systematic review in the International Journal of Otolaryngology and Head & Neck Surgery (Ganchi, 2025), stem cell therapy shows promise for potentially curing congenital hearing loss via cochlear regeneration. However, significant hurdles in protocol development, long-term efficacy, and safety must still be addressed.
Conclusion
Recent developments in stem cell trials are shifting the treatment of tinnitus and neural hearing loss toward addressing the underlying damage rather than just managing symptoms. While still in trials, these regenerative therapies could significantly change the landscape of hearing restoration.

 By Gazette Staff By Gazette Staff
September 15th, 2025
BURLINGTON, ON
Five Halton residents have tested positive for West Nile virus. These are the first human cases for Halton this year.
“Halton Region Public Health works to reduce the risk of West Nile virus in our community through both education and preventative programs such as larviciding.
Until the fall frost, Halton residents should continue to protect themselves and their families against mosquito bites and remove mosquito breeding sites,” said Dr. Patrick Galange, Halton Region Associate Medical Officer of Health. “About 80 per cent of individuals infected with West Nile virus will have no symptoms, while some may develop fever, headache, body aches, joint pains, vomiting, diarrhea or rash. About one in a hundred people infected with West Nile virus may develop a severe illness affecting the central nervous system. This may present as encephalitis (inflammation of the brain) or meningitis (inflammation of the membranes that surround the brain and spinal cord).”
 Protect yourself and your family from mosquitoes by: Protect yourself and your family from mosquitoes by:
-
Covering up when going outside between the hours of dusk and dawn (when most mosquitoes feed), and at any time in shady, wooded areas. Wear light-coloured, long-sleeved shirts and pants with tightly-woven fabric.
Using an approved insect repellent, such as one containing DEET or Icaridin.
Reducing mosquito-breeding sites around your home by getting rid of all water-filled containers and objects, where possible. Change the water in bird baths at least once per week.
Making sure your window and door screens are tight and without holes, cuts or other openings.
To learn more about personal protection and Halton Region’s surveillance and control efforts, visit the West Nile Virus page on halton.ca. To report standing water on public property, call 311.

 By Gazette Staff By Gazette Staff
August 29th, 2025
BURLINGTON, ON
 The Ontario Health Coalition has been fighting the good fight to keep the health service public and not something that drifts into the hands of the private sector. The Ontario Health Coalition has been fighting the good fight to keep the health service public and not something that drifts into the hands of the private sector.
They have been demonstrating across the province and documenting the number of emergency rooms that are closed and small communities that find they no longer have access to the health services.
They are circulating a petition to collect signatures from people who want to see a stop to the closings that are taking place.

The group continues to tell the story of what is taking place.
Public hospitals’ operating rooms idle while patients wait
Our public hospitals’ operating rooms are closed evenings, weekends– some even permanently. They aren’t given enough funding to run full time, which would reduce waitlists.
Record emergency department closures
Ontario had more than 1,100 emergency department closures last year. Local hospitals, in existence for 100 years, are now at risk of permanent closures. If the Ford government chose, they could restore services by funding & staffing our public hospitals.
Lowest public hospital funding while $ billions shifted to private health care
Ontario funds our public hospitals at the lowest rate of any province. At the same time, the Ford government is redirecting more than a billion dollars per year from our public taxes to fund private for-profit clinics & staffing corporations.
For-profit clinics charge patients $$ thousands in illegal (& unethical) user fees for surgeries & tests
Maureen needed eye surgery for macular degeneration so she wouldn’t lose her vision. A private clinic charged her $7,000. She told us, “Being a senior on a fixed income, I’m still trying to catch up with my bills from the surgery.”
This should NEVER happen. The Ontario government is responsible for enforcing our medicare laws to protect patients like Maureen from extra-billing & user fees. Medically needed surgeries & tests must be covered by OHIP. That’s the law.
Last spring, we made a complaint to the Ford government from 50 patients – including Maureen – who were charged or manipulated into paying for medically unnecessary add ons in private clinics. The patients should be reimbursed & the clinics should be stopped.
We’re making another complaint this fall to push the Ford government to stop them. If you’ve been charged for your surgery, please contact us.
Ontario has downsized our hospitals to an extreme extent.
We are last in Canada & third from the bottom among developed nations.
 In 1990, Ontario had 50,000 hospital beds for 10.3 million people. Today, we only have 35,000 for 16.2 million people. In 1990, Ontario had 50,000 hospital beds for 10.3 million people. Today, we only have 35,000 for 16.2 million people.
According to data from the OECD, only Chile & Mexico have fewer hospital beds per person than Ontario.
Why? Because everything they cut from public hospitals is privatized.
NOTE: A “hospital bed” means a bed that is funded with nurses, doctors & other staff providing care. When they close down “beds” it means they cut staff & the care they provide. Patients are backlogged in emergency departments because they are waiting for a funded bed to open up for them inside the hospital, while thousands of beds have been closed down & could be reopened.
Please send a message to Doug Ford: You can’t say you stand up for Canada while privatizing our health care
The United States has the most privatized health care in the developed world. Americans pay almost double our costs for care.
The Ford government is privatizing more & more of our long-term care and hospital surgeries & diagnostics. They’re giving primary care to for-profit chains, privatizing Public Health services like COVID testing, vaccines & more. They’re allowing private clinics to bill OHIP & charge patients on top. They’re moving toward U.S.-style for-profit health care.
U.S. for-profit hospitals charge exorbitant prices. Businesses face high insurance costs for employees. On top, employees pay co-payments every paycheque plus they have to pay deductibles before coverage kicks in…IF they are covered. Insurance companies make profits by denying coverage.
Medical costs are the top reason for bankruptcy: 56 million Americans struggle with medical debt: more than Canada’s entire population.
Every one of us can make a difference

 By Gazette Staff By Gazette Staff
August 27th, 2025
BURLINGTON, ON
UPDATE from the Ministry of Health: Following regulatory amendments made under the Pharmacy Act, pharmacy professionals are now authorized to administer the RSV vaccine.
While pharmacists are authorized to administer the adult RSV vaccine in Ontario, pharmacists do not have direct access to the publicly funded RSV vaccine supply.
The Ontario government is expanding the Respiratory Syncytial Virus (RSV) prevention program to include all individuals aged 75 years and older, helping to protect those most vulnerable during the upcoming respiratory illness season.
The media release did not say how the immunization would be delivered – we are following up on that.
 RSV prevention program to include all individuals aged 75 years and older, helping to protect those most vulnerable during the upcoming respiratory illness season. “Our government is ensuring the most vulnerable have access to the tools they need to protect themselves and their family during respiratory illness season,” said Sylvia Jones, Deputy Premier and Minister of Health. “We’re once again expanding RSV immunization which will now include everyone 75 years of age and older so we can help protect more seniors and reduce unnecessary hospitalizations this fall and winter.”
Starting this fall, RSV immunization will now be available through Ontario’s publicly funded RSV immunization programs to all individuals aged 75 and older, building on last year’s expansion of the programs that also includes:
-
Certain high-risk adults aged 60 to 74, such as residents of long-term care homes or retirement homes
Infants up to eight months of age in their first RSV season
High-risk children up to 24 months of age in their second season
Pregnant women will have the option to receive the RSV vaccine Abrysvo®, which can help provide protection to infants at birth, while eligible newborns, infants and high-risk children can receive the Beyfortus® immunization. More details on where families will be able to access RSV immunization will be provided in the coming weeks.
“As we prepare for the upcoming respiratory illness season, it’s essential that we take proactive steps to protect those most at risk and reduce pressure on our health-care system,” said Dr. Kieran Moore, Ontario’s Chief Medical Officer of Health. “Ontario’s RSV immunization programs for infants, high-risk children, high-risk adults over 60 and everyone aged 75 and older is a critical part of our strategy to prevent severe illness, hospitalizations, and complications, especially among those most vulnerable to respiratory infections.”
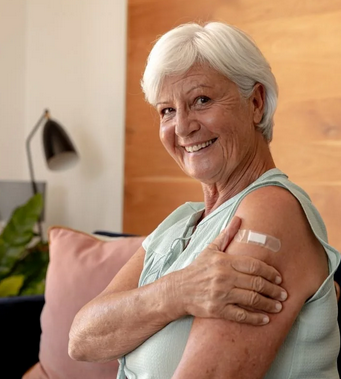 Routine and recommended immunizations help prevent the spread of serious diseases throughout communities. Routine and recommended immunizations help prevent the spread of serious diseases throughout communities, reduce medical visits and keep people out of the hospital. Everyone is strongly encouraged to stay up to date on their immunizations, especially children returning to school who may have missed routine vaccines.
Through Your Health: A Plan for Connected and Convenient Care, the Ontario government is providing people with the tools they need to connect to the care they need to keep themselves and their loved ones safe and healthy.
Quick Facts
-
Information about recommended immunizations for the upcoming respiratory illness season, including when to get your flu shot and COVID-19 vaccine, will be available closer to the fall.
Respiratory Syncytial Virus (RSV) is a common respiratory virus that infects the nose, throat, and lungs. Infection is most severe in young babies and older adults and can cause serious lung infections that may require hospitalization. RSV infection can also make chronic health problems worse.
Pregnant women should consult with their health-care provider before receiving Abrysvo®.
Every time your child gets a routine immunization, report it to your local public health unit to ensure their records for the ISPA are up to date. Health-care providers do not report these records for you.
Under Ontario’s Immunization of School Pupils Act (ISPA), students must provide proof of immunization against diseases such as measles, mumps, rubella and whooping cough to attend school.
Talk to a health-care provider or public health unit if you are unsure if your child has missed routine immunizations or if you are unsure about which immunizations they have received.
Visit Health811 online or call 811 (TTY: 1-866-797-0007 toll free) for health advice and information 24 hours a day, seven days a week.

 By Gazette Staff By Gazette Staff
August 13th, 2025
BURLINGTON, ON
What if a simple heartbeat measurement could help predict a person’s risk of dementia?
A Brock-led international research team has found that including an additional metric — resting heart rate — to an established dementia risk prediction model can make its results more accurate across most racial groups, says Professor of Health Sciences Newman Sze.
The Cardiovascular Risk Factors, Aging and Incidence of Dementia (CAIDE) international assessment tool uses several physiological and social measurements to evaluate a patient’s vulnerability to developing dementia in the future.
 But the current model doesn’t capture a patient’s full health picture, particularly across diverse racial groups in the U.S., says Sze, the Canada Research Chair in Mechanisms of Health and Disease. But the current model doesn’t capture a patient’s full health picture, particularly across diverse racial groups in the U.S., says Sze, the Canada Research Chair in Mechanisms of Health and Disease.
After obesity and hypertension, Sze says resting heart rate is one of the most important risk factors for dementia, a feature not captured in the current model.
“If the resting heart rate is too low or too fast due to heart muscle failure, there’s not enough blood being pumped to the brain,” says Sze. “The brain doesn’t receive enough oxygen and nutrients, which leads to brain degeneration.”
Sze and his eight-member research team tested the impacts of including resting heart rate (RHR) in the CAIDE model to see if adding that measurement would improve the model as a whole and increase equitable access to dementia prediction.
Resting heart rate, or pulse rate, refers to the number of beats per minute when the body is inactive and calm.
 The research team analyzed data from 44,467 U.S. participants aged 18 and older, including those aged 65 and above. The data, collected by the National Alzheimer’s Coordinating Center (NACC), spanned from 2005 to 2023 and included information from interviews, physical examinations and cognitive tests. The research team analyzed data from 44,467 U.S. participants aged 18 and older, including those aged 65 and above. The data, collected by the National Alzheimer’s Coordinating Center (NACC), spanned from 2005 to 2023 and included information from interviews, physical examinations and cognitive tests.
The team divided participants in the NACC database into self-reported racial groups: two American Indigenous populations, Asian, Black African, Hispanic and White.
The team ran each group through the current CAIDE model, which is comprised of age, sex, body mass index, hypercholesteremia, level of education and hypertension measurements.
They then repeated the procedure with a CAIDE-RHR model that included resting heart rate.
“This adjustment significantly improved dementia risk prediction across most racial groups, offering a more inclusive and accessible way to identify at-risk individuals,” says Sze.
As resting heart rate is easy to measure, more people can be screened and monitored, which makes the model more inclusive, says the study’s lead author, PhD student Shakiru Alaka.
He says other researchers have previously attempted to improve the CAIDE model’s accuracy by introducing expensive and time-consuming lab analysis to detect dementia biomarkers in blood samples.
But this addition may reduce access for multi-racial, underserved populations, especially in the U.S., says Alaka.
“In contrast, resting heart rate can be measured with a simple blood pressure cuff or by placing fingers on the wrist — methods that are quick, non-invasive and widely available, even in underserved community settings,” he says.
The team found the CAIDE-RHR model significantly improved the accuracy of dementia risk prediction for all racial groups in the study except the American Indigenous populations, although Sze says the low number of participants may have affected the model’s accuracy for that group.
“This finding highlights the important connection between heart health and brain health,” says Sze. “It’s a step toward addressing systemic gaps in how we assess dementia risk across diverse populations.”
 Newman Sze and PhD student Shakiru Alaka checking data at Brock University Although the study was conducted with U.S. participants, the findings have important implications for Canada, where dementia-related mortality has increased by 59 per cent over the past 10 years, says Sze.
“The CAIDE-RHR model offers a low-cost, non-invasive tool that could be integrated into routine care, including in rural and underserved communities, to help identify those at risk earlier and more equitably,” he says.
The study, “Enhancing the Validity of CAIDE Dementia Risk Scores with Heart Rate and Machine Learning: An Analysis from National Alzheimer Coordinating Centre Across All Races/Ethnicity,” was published Friday, Aug. 8 in Alzheimer’s & Dementia: The Journal of the Alzheimer’s Association.
In addition to Sze and Alaka, the research team includes Brock University Professor of Health Sciences Brent Faught, Distinguished Professor of Kinesiology Panagiota Klentrou, Associate Professor of Health Sciences Rebecca MacPherson, Assistant Professor of Health Sciences Mostafa Shokoohi, Research Associate So-Fong Cam Ngan and researchers from the U.K.’s Newcastle University and the National University Health System in Singapore.

 By Gazette Staff By Gazette Staff
April 10th, 2025
BURLINGTON, ON
Halton Region Public Health has issued an Extended Heat Warning starting August 11, 2025 for Halton Region as a result of Environment Canada continuing its Heat Warning. An Extended Heat Warning is issued when the daytime temperatures are expected to reach at least 31 degrees Celsius with overnight temperatures above 20 degrees Celsius for three or more days, or when the humidex is expected to reach 40 for three or more days.
 Heat stroke is a medical emergency. Exposure to these weather conditions can cause serious health problems those especially at risk include: older adults, infants and young children, people who work and exercise in the heat, people without adequate housing and those without air conditioning. People who have breathing difficulties, heart problems, kidney problems or are taking medication that affect their sensitivity to heat are also especially at risk of preventable heat illness. This warning is intended to inform the general public and community agencies, to keep residents safe and healthy during the heat and to recommend that precautions are taken when temperatures are high.
As the climate changes, heat events are expected to become more frequent, longer and hotter in Halton Region and other parts of Ontario.
Heat stroke is a medical emergency. Call 911 if you are caring for someone who has a high body temperature and is either unconscious, confused or has stopped sweating. Cool the person as best you can while waiting for medical attention to arrive.
You can prevent heat-related illnesses by avoiding strenuous outdoor activities; seeking shade from the sun; spending time in air-conditioned places, such as shopping malls and community centres; and staying hydrated. Call or visit friends and neighbours who may be at risk and never leave people or pets in your care unattended in a car.
Weather and heat information are available on local radio and television stations and the Environment Canada Weather Conditions and Forecast webpage. Also, check the Air Quality Health Index, air pollution tends to be higher during very hot days. For information and tips on how to protect your health during heat warnings, including information on cooling centres, please visit our Preparing for Heat Events webpage at halton.ca or call 311.

 By Aria Wilson By Aria Wilson
July 31st, 2025
BURLINGTON ON
Our world is a changing place. With the introduction of mental health destigmatization comes tough realities. This is one of many stories of a family changed by the devastating impacts of negative mental health. This is the story of my family.
It was the end of the school year in 2020. I thought that I was just going to get a two-week break from school. While I enjoyed the time spent online, playing games with my friends, it never occurred to me that the adults and loved ones in my life were slowly beginning to feel more alone, more isolated from the world around them. With the virtual shift caused by the COVID-19 pandemic came job losses and a decline in communication with people who you loved. Sometimes a difference of opinion was enough to tear people apart at such a troubling time.
I often come back to the pandemic when I think of the causes of the uptick in mental health problems lately, especially in more mature demographics. According to the World Health Organization, global levels of anxiety and depression increased twenty-five per cent in the first year of the pandemic. I wonder if perhaps the lack of in-person interaction was enough to cause some of the cases. I know that this certainly contributed to my story.
 It wasn’t until a couple of years later that the problems for my family came to the surface. At this time, a member of my family had already been struggling with his physical health for several years. He had slipped a disc in his spine, a painful and debilitating injury. Through countless doctor’s visits, several neurology appointments, and seemingly endless surgeon consults, nothing had been done to change the situation this individual faced. It wasn’t until a couple of years later that the problems for my family came to the surface. At this time, a member of my family had already been struggling with his physical health for several years. He had slipped a disc in his spine, a painful and debilitating injury. Through countless doctor’s visits, several neurology appointments, and seemingly endless surgeon consults, nothing had been done to change the situation this individual faced.
Due to hospital systems being overworked and overbooked, surgery continuously got pushed further. The longer we waited, the more it started to feel like we would never get the chance to see change. I think this is when my family member’s mental health began to dwindle.
Losing hope by the minute, there seemed to be very little that could be done for our family. Other than occasional spinal injections that do little but numb the spine, mobility became even more of a challenge and limited this individual’s connection to the world.
 Left: Eric Vandewall, president and CEO of Joseph Brant Hospital; Michael Paletta; launched the For All Minds campaign with a $5-million donation from Michael and Laura Paletta towards a $20-million community fundraising goal. It all came to a head when my family member was admitted to the hospital in the Inpatient Mental Health Unit. With all the physical strain that had not been resolved, a mental toll had ultimately overtaken the problems plaguing my family member.
The first time we admitted him to the hospital, he only spent a night before he came home. I believe this was a mistake, as he had to return to the hospital no more than a week later.
While the programs available in the hospital were helpful during his stay, we found little communication and follow-up after his visits, leading to a cycle of short stays at home, followed by the necessity to return to the hospital.
We have finally, after more than five stays in the mental health unit, found a day program to assist the family member’s mental health. And still, to this day, he has not received any notice of available surgery for mobility complications.
I do not place blame on the hospital systems; I know that staff have truly cared for my family and want to see my family member get better.
If nothing, let my story serve as a reminder to spend time with your family, teach them new ways to interact with each other and stay active, and certainly don’t take any of your time together for granted.
 Aria Wilson will return to Carlton University in September to begin her second year as a journalism student Aria Wilson will return to Carlton University in September to begin her second year as a journalism student

|
|
 By Gazette Staff
By Gazette Staff Irene Matys is a World Gourmand Award winning and Globe and Mail bestselling cookbook author, television food expert, and farm-to-table advocate. She is the author of My Cypriot Table: Mediterranean Recipes for Gathering, Sharing, and Savouring, a celebrated debut cookbook featuring over 100 vibrant recipes inspired by her Greek Cypriot heritage and Canada’s seasonal bounty.
Irene Matys is a World Gourmand Award winning and Globe and Mail bestselling cookbook author, television food expert, and farm-to-table advocate. She is the author of My Cypriot Table: Mediterranean Recipes for Gathering, Sharing, and Savouring, a celebrated debut cookbook featuring over 100 vibrant recipes inspired by her Greek Cypriot heritage and Canada’s seasonal bounty.













 By Gazette Staff
By Gazette Staff
 On Monday March 16, people across Canada rallied outside the offices of their local Liberal Members of Parliament in a nationwide Day of Action to warn that public health care for all in Canada is under unprecedented threat and to call on the federal government to enforce the Canada Health Act. The Ontario Health Coalition held seven events in Ontario in Ajax, Hamilton, London, Peterborough, Toronto and Waterloo — and one more is coming up in Kingston on Friday, March 20 at t
On Monday March 16, people across Canada rallied outside the offices of their local Liberal Members of Parliament in a nationwide Day of Action to warn that public health care for all in Canada is under unprecedented threat and to call on the federal government to enforce the Canada Health Act. The Ontario Health Coalition held seven events in Ontario in Ajax, Hamilton, London, Peterborough, Toronto and Waterloo — and one more is coming up in Kingston on Friday, March 20 at t By Gazette Staff
By Gazette Staff In November 2025, Mr. Allen received a letter from Halton Region Public Health advising that improper infection prevention and control practices involving the use of unsterile needles with multidose vials of anesthetic medication had been identified at the clinic. The letter advised him to consult his healthcare provider and undergo testing for Hepatitis B, Hepatitis C and HIV.
In November 2025, Mr. Allen received a letter from Halton Region Public Health advising that improper infection prevention and control practices involving the use of unsterile needles with multidose vials of anesthetic medication had been identified at the clinic. The letter advised him to consult his healthcare provider and undergo testing for Hepatitis B, Hepatitis C and HIV. The lawsuit alleges the defendants breached their duty of care by failing to implement appropriate infection prevention and control measures and failing to ensure needles used in treatment were properly sterilized. The lawsuit also alleges Halton Family Health Centre Inc. is vicariously liable for the conduct of Dr. Salter.
The lawsuit alleges the defendants breached their duty of care by failing to implement appropriate infection prevention and control measures and failing to ensure needles used in treatment were properly sterilized. The lawsuit also alleges Halton Family Health Centre Inc. is vicariously liable for the conduct of Dr. Salter. By Lori Croonen
By Lori Croonen 






 By Gazette Staff
By Gazette Staff “Statistically, we see a rise in heart attacks and heart-related deaths after significant snowfalls,” says Dr. Craig Ainsworth, Cardiology and Chief of Critical Care at Hamilton Health Sciences’ Hamilton General Hospital (HGH). “Repeatedly lifting heavy snow causes your heart rate to increase and blood pressure to rise considerably. For some people, especially those with certain risk factors, this can lead to a heart attack.”
“Statistically, we see a rise in heart attacks and heart-related deaths after significant snowfalls,” says Dr. Craig Ainsworth, Cardiology and Chief of Critical Care at Hamilton Health Sciences’ Hamilton General Hospital (HGH). “Repeatedly lifting heavy snow causes your heart rate to increase and blood pressure to rise considerably. For some people, especially those with certain risk factors, this can lead to a heart attack.”
 By Gazette Staff
By Gazette Staff The measles outbreak in Canada and how we reacted to it has resulted in the Pan American Health Organization (PAHO) advising the The Public Health Agency of Canada that it has lost its measles elimination status — a designation it has held since 1998.
The measles outbreak in Canada and how we reacted to it has resulted in the Pan American Health Organization (PAHO) advising the The Public Health Agency of Canada that it has lost its measles elimination status — a designation it has held since 1998.
 By Pepper Parr
By Pepper Parr University Professor Tim O’Connell, Chair of Recreation and Leisure Studies at Brock University explains that: “As society increasingly embraces a holistic approach to health, recreation has emerged at the critical intersection of personal wellness and community well-being.
University Professor Tim O’Connell, Chair of Recreation and Leisure Studies at Brock University explains that: “As society increasingly embraces a holistic approach to health, recreation has emerged at the critical intersection of personal wellness and community well-being.
 This public notice has been updated to provide clarity and ensure an accurate understanding of the infection prevention and control lapse. It is important to note that the same needle was not used continuously throughout the period, rather appropriate infection prevention and control measures were not followed when using multi does vials over the time period identified.
This public notice has been updated to provide clarity and ensure an accurate understanding of the infection prevention and control lapse. It is important to note that the same needle was not used continuously throughout the period, rather appropriate infection prevention and control measures were not followed when using multi does vials over the time period identified. By Gazette Staff
By Gazette Staff

 By Gazette Staff
By Gazette Staff Protect yourself and your family from mosquitoes by:
Protect yourself and your family from mosquitoes by: The Ontario Health Coalition has been fighting the good fight to keep the health service public and not something that drifts into the hands of the private sector.
The Ontario Health Coalition has been fighting the good fight to keep the health service public and not something that drifts into the hands of the private sector.
 In 1990, Ontario had
In 1990, Ontario had 

 The research team analyzed data from 44,467 U.S. participants aged 18 and older, including those aged 65 and above. The data, collected by the National Alzheimer’s Coordinating Center (NACC), spanned from 2005 to 2023 and included information from interviews, physical examinations and cognitive tests.
The research team analyzed data from 44,467 U.S. participants aged 18 and older, including those aged 65 and above. The data, collected by the National Alzheimer’s Coordinating Center (NACC), spanned from 2005 to 2023 and included information from interviews, physical examinations and cognitive tests.
 By Gazette Staff
By Gazette Staff
 By Aria Wilson
By Aria Wilson It wasn’t until a couple of years later that the problems for my family came to the surface. At this time, a member of my family had already been struggling with his physical health for several years. He had slipped a disc in his spine, a painful and debilitating injury. Through countless doctor’s visits, several neurology appointments, and seemingly endless surgeon consults, nothing had been done to change the situation this individual faced.
It wasn’t until a couple of years later that the problems for my family came to the surface. At this time, a member of my family had already been struggling with his physical health for several years. He had slipped a disc in his spine, a painful and debilitating injury. Through countless doctor’s visits, several neurology appointments, and seemingly endless surgeon consults, nothing had been done to change the situation this individual faced.
 Aria Wilson will return to Carlton University in September to begin her second year as a journalism student
Aria Wilson will return to Carlton University in September to begin her second year as a journalism student